|
![]()
| A potentially unsustainable financial burden on the health system What1 #348767 The range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050). | Simon Stevens, Chief Executive of NHS England warned in September 2014 of the need to get serious about obesity or bankrupt the NHS (with the cost of treating the health consequences of obesity escalating as the prevalence of obesity spreads in the population): Obesity is the new smoking, and it represents a slow-motion car crash in terms of avoidable illness and rising health care costs... If as a nation we keep piling on the pounds around the waistline, we’ll be piling on the pounds in terms of future taxes needed just to keep the NHS afloat. [13] The McKinsey Global Institute analysis [11] found that obesity generated an economic loss in the UK of more than $70 billion a year in 2012, or 3.0 percent of GDP (see below); the second biggest impact – within the analysis as defined (covering the loss of productive life, direct health-care costs, and investment to mitigate the cost) – of 14 human generated burdens: 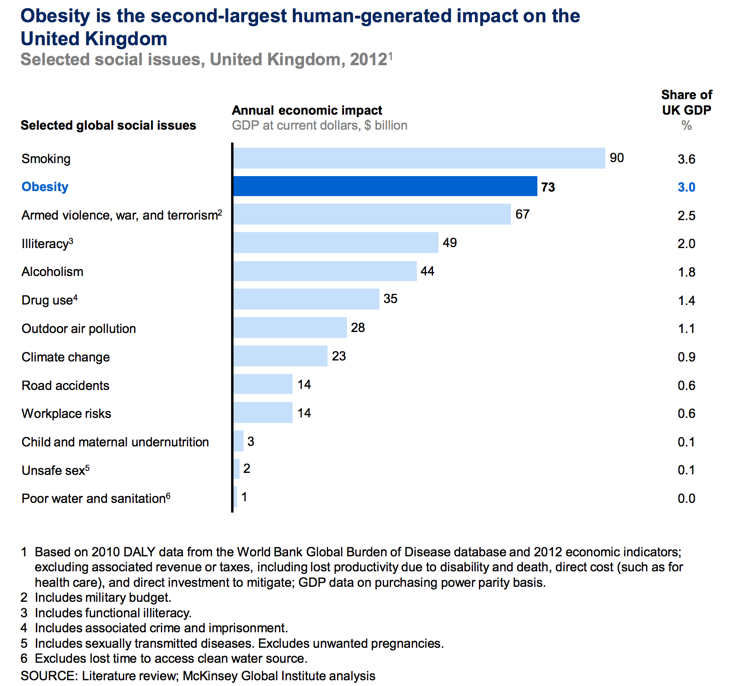
Source: McKinsey Global Institute A 2010 review by the National Obesity Observatory of previous economic analyses of the burden of obesity in the UK noted: [2] - Estimates of the direct NHS costs of treating overweight and obesity, and related morbidity in England have ranged from £479.3m in 1998 [4] to £4.2bn in 2007. [1]
- Estimates of the indirect costs (those costs arising from the impact of obesity on the wider economy such as loss of productivity) from these studies ranged between £2.6bn [4] and £15.8 billion.[1] Modelled projections suggest that indirect costs could be as much as £27bn by 2015. In 2006/07, obesity and obesity-related illness was estimated to have cost £148 million in inpatient stays in England. [10]

Source: Foresight Report, 2007 - Premature deaths attributable to obesity lead to the annual loss of around 45,000 years of working life. Sickness absence attributable to obesity is estimated at between 15.5 million and 16 million days per year.Obese people are much less likely to be in employment than those of healthy weight, with associated welfare costs estimated at between £1 billion and £6 billion. The total cost to the economy of being overweight or obese has been estimated as some £16 billion in 2007, rising to £50 billion per year by 2050 if left unchecked.
- It is estimated that 23% of spending on all drugs is attributable to overweight and obesity. The minimum annual cost of any drug prescriptions at BMI 20 rose from £50.71 for men and £62.59 for women by £5.27 and £4.20, respectively, for each unit increase in BMI to a BMI of 25.3 Increases for each BMI unit were greater to BMI 30, and greater still, £8.27 (men) and £4.95 (women), to BMI 40.

Source: Foresight Report, 2007 |
+Citations (14) - CitationsAjouter une citationList by: CiterankMapLink[1] Foresight Report - Tackling obesities: future choices – project report (2nd Ed)
En citant: Bryony Butland et al. - Government Office for Science
Publication info: 2007 October, 17
Cité par: David Price 8:46 AM 28 July 2014 GMT
Citerank: (28) 340964Tackling obesity in the UKWith concern growing that the Foresight analysis—that 50% of the UK population could be obese by 2050, at an annual cost to the nation of around £50 billion per year [2]—substantially underestimates the scale of the unfolding obesity crisis, the College of Contemporary Health is working with the wider policy community to develop a whole systems map of the obesity crisis and the potential responses.7F1CEB7, 348675Adopt a whole systems approach to obesityTackling obesity effectively—accomplishing a population wide-shift—requires a comprehensive and integrated whole systems approach, involving a range of measures focusing on individuals, social and other systems, including at the local and community level, and on the interrelated physical, physiological, social and cognitive factors that determine health outcomes.565CA4D9, 348688Impacts of obesityObesity presents a significant threat to the health of the UK population and a significant drain on the nation's financial resources. 24.9% of adults in England are obese—with a body mass index of over 30—62% of adults are either overweight or obese (with a BMI of over 25), and 32% of 10–11-year-olds are overweight or obese. The annual cost of obesity to the UK is estimated to be £27bn–£46bn [1], [2]; although international comparisons suggest that the true cost could be significantly higher.57DE7179, 348693Stakeholders – Groups & ActionsExplore the map via the different stakeholder groups and the measures each group can take to help tackle the obesity crisis.58D3ABAB, 348770Tackling obesityMany policy interventions have been suggested to address the obesity crisis across multiple studies—and indeed many such measures have been implemented, and are being implemented, now. There's recognition too that these interventions need to be part of a coherent and comprehensive whole systems strategy [4]; with some grounds for optimism that such an approach has the potential to accomplish a significant reduction in the prevalence of obesity in the UK across the next decade. [2]565CA4D9, 348775Modelling suggests the majority of UK population may be obese by 2050The prevalence of obesity in the UK more than doubled in the 25 years to 2007. In England, nearly a quarter of adults and about 10% of children were obese in 2007, with a further 20–25% of children overweight. The Foresight report extrapolated that 40% of Britons might be being obese by 2025, with Britain being a mainly obese society by 2050.1198CE71, 348776A profound impact on the health of the populationObesity is responsible for more than 9,000 premature deaths each year in England, reduces life expectancy on average by nine years, and is a major risk factor in wide range of serious health problems including Type 2 diabetes (5 x), cancer (3 x the risk of colon cancer), and heart disease (2.5 x).57DE7179, 348779Involve all stakeholders in the process of changeReversing the rising trend and addressing the prospect of the rising health burden and societal costs will be demanding and will necessitate major changes in behaviour – not only in individuals, but also in families, communities, organisations and economic markets.565CA4D9, 348780Causes of obesityUnderstanding the causes of obesity is critical to the success of prevention and treatment strategies. However, while (simply put) obesity occurs when energy intake from food and drink consumption is greater than energy expenditure through the body’s metabolism and physical activity over a prolonged period (resulting in the accumulation of excess body fat), in reality many complex behavioural and societal factors contribute systemically to the current crisis and no single influence dominates.555CD992, 351674Inequality of impactAlthough obesity occurs across all population groups, it impacts disproportionately on the socially and economically disadvantaged and some ethnic minorities. [8]57DE7179, 352390Industrial way of life is obesogenicRapid societal changes—for example, in food production, motorised transport and work/home lifestyle patterns—have placed human physiology (which has evolved to cope with an under-supply of food and high energy expenditure) under new stresses, and revealed an underlying genetic tendency to accumulate and conserve energy (i.e. gain weight) in a high proportion of the population. In this sense, obesity can be construed as a normal physiological response to an abnormal environment.555CD992, 352390Industrial way of life is obesogenicRapid societal changes—for example, in food production, motorised transport and work/home lifestyle patterns—have placed human physiology (which has evolved to cope with an under-supply of food and high energy expenditure) under new stresses, and revealed an underlying genetic tendency to accumulate and conserve energy (i.e. gain weight) in a high proportion of the population. In this sense, obesity can be construed as a normal physiological response to an abnormal environment.555CD992, 365986Foresight – Obesity System MapObesity occurs when energy intake from food and drink consumption is greater than energy expenditure through the body’s metabolism and physical activity over a prolonged period, resulting in the accumulation of excess body fat. However there are many complex behavioural and societal factors that combine to contribute to the causes of obesity.7F1CEB7, 366467Encourage active transport (walking and cycling)Government authorities redesign urban planning to facilitate and encourage walking and cycling.565CA4D9, 366990What costs should be included in the financial analysis?What cost factors should be included in the assessment of the overall financial impact of obesity on the UK economy?8FFB597, 399546Tackling obesityMany policy interventions have been suggested to address the obesity crisis across multiple studies—and indeed many such measures have been implemented, and are being implemented, now. There's recognition too that these interventions need to be part of a coherent and comprehensive whole systems strategy [4]; with some grounds for optimism that such an approach has the potential to accomplish a significant reduction in the prevalence of obesity in the UK across the next decade. [2]565CA4D9, 399547Adopt a whole systems approach to obesityTackling obesity effectively—accomplishing a population wide-shift—requires a comprehensive and integrated whole systems approach, involving a range of measures focusing on individuals, social and other systems, including at the local and community level, and on the interrelated physical, physiological, social and cognitive factors that determine health outcomes.565CA4D9, 399557Involve all stakeholders in the process of changeReversing the rising trend and addressing the prospect of the rising health burden and societal costs will be demanding and will necessitate major changes in behaviour – not only in individuals, but also in families, communities, organisations and economic markets.565CA4D9, 399599Encourage active transport (walking and cycling)Government authorities redesign urban planning to facilitate and encourage walking and cycling.565CA4D9, 399887Causes of obesityUnderstanding the causes of obesity is critical to the success of prevention and treatment strategies. However, while (simply put) obesity occurs when energy intake from food and drink consumption is greater than energy expenditure through the body’s metabolism and physical activity over a prolonged period (resulting in the accumulation of excess body fat), in reality many complex behavioural and societal factors contribute systemically to the current crisis and no single influence dominates.555CD992, 399889Industrial way of life is obesogenicRapid societal changes—for example, in food production, motorised transport and work/home lifestyle patterns—have placed human physiology (which has evolved to cope with an under-supply of food and high energy expenditure) under new stresses, and revealed an underlying genetic tendency to accumulate and conserve energy (i.e. gain weight) in a high proportion of the population. In this sense, obesity can be construed as a normal physiological response to an abnormal environment.555CD992, 399889Industrial way of life is obesogenicRapid societal changes—for example, in food production, motorised transport and work/home lifestyle patterns—have placed human physiology (which has evolved to cope with an under-supply of food and high energy expenditure) under new stresses, and revealed an underlying genetic tendency to accumulate and conserve energy (i.e. gain weight) in a high proportion of the population. In this sense, obesity can be construed as a normal physiological response to an abnormal environment.555CD992, 399972Impacts of obesityObesity presents a significant threat to the health of the UK population and a significant drain on the nation's financial resources. 23% of adults are obese—with a body mass index of over 30—61% of adults are either overweight or obese (with a BMI of over 25), and 33% of 10–11-year-olds are overweight or obese. The annual cost of obesity to the UK economy has been estimated to be £27bn–£46bn [1], [2]; although international comparisons suggest that the true cost could be significantly higher.57DE7179, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179, 399974A profound impact on the health of the populationObesity is responsible for more than 9,000 premature deaths each year in England, reduces life expectancy on average by nine years, and is a major risk factor in wide range of serious health problems including Type 2 diabetes (5 x), cancer (3 x the risk of colon cancer), and heart disease (2.5 x).57DE7179, 399978Modelling suggests the majority of UK population may be obese by 2050The prevalence of obesity in the UK more than doubled in the 25 years to 2007. In England, nearly a quarter of adults and about 10% of children were obese in 2007, with a further 20–25% of children overweight. The Foresight report extrapolated that 40% of Britons might be being obese by 2025, with Britain being a mainly obese society by 2050.1198CE71, 399980What costs should be included in the financial analysis?What cost factors should be included in the assessment of the overall financial impact of obesity on the UK economy?8FFB597, 399984Inequality of impactAlthough obesity occurs across all population groups, it impacts disproportionately on the socially and economically disadvantaged and some ethnic minorities. [8]57DE7179 URL:
| | Extrait - The rapid increase in the number of obese people in the UK is a major challenge. This analysis by the government’s Foresight programme shows that over half of the UK adult population could be obese by 2050. The economic implications are substantial. The NHS costs attributable to overweight and obesity are projected to double to £10 billion per year by 2050. The wider costs to society and business are estimated to reach £49.9 billion per year (at today’s prices). |
Link[3] Preventing Obesity – A Whole-System Approach
En citant: National Institute for Health and Care Excellence
Publication info: 2010
Cité par: David Price 12:22 PM 1 September 2014 GMT
Citerank: (11) 348675Adopt a whole systems approach to obesityTackling obesity effectively—accomplishing a population wide-shift—requires a comprehensive and integrated whole systems approach, involving a range of measures focusing on individuals, social and other systems, including at the local and community level, and on the interrelated physical, physiological, social and cognitive factors that determine health outcomes.565CA4D9, 348688Impacts of obesityObesity presents a significant threat to the health of the UK population and a significant drain on the nation's financial resources. 24.9% of adults in England are obese—with a body mass index of over 30—62% of adults are either overweight or obese (with a BMI of over 25), and 32% of 10–11-year-olds are overweight or obese. The annual cost of obesity to the UK is estimated to be £27bn–£46bn [1], [2]; although international comparisons suggest that the true cost could be significantly higher.57DE7179, 348780Causes of obesityUnderstanding the causes of obesity is critical to the success of prevention and treatment strategies. However, while (simply put) obesity occurs when energy intake from food and drink consumption is greater than energy expenditure through the body’s metabolism and physical activity over a prolonged period (resulting in the accumulation of excess body fat), in reality many complex behavioural and societal factors contribute systemically to the current crisis and no single influence dominates.555CD992, 351674Inequality of impactAlthough obesity occurs across all population groups, it impacts disproportionately on the socially and economically disadvantaged and some ethnic minorities. [8]57DE7179, 351678Key questions for a whole systems approachA set of key questions for a whole systems approach identified by the National Institute for Health and Care Excellence.8FFB597, 399547Adopt a whole systems approach to obesityTackling obesity effectively—accomplishing a population wide-shift—requires a comprehensive and integrated whole systems approach, involving a range of measures focusing on individuals, social and other systems, including at the local and community level, and on the interrelated physical, physiological, social and cognitive factors that determine health outcomes.565CA4D9, 399746Key questions for a whole systems approachA set of key questions for a whole systems approach identified by the National Institute for Health and Care Excellence.8FFB597, 399887Causes of obesityUnderstanding the causes of obesity is critical to the success of prevention and treatment strategies. However, while (simply put) obesity occurs when energy intake from food and drink consumption is greater than energy expenditure through the body’s metabolism and physical activity over a prolonged period (resulting in the accumulation of excess body fat), in reality many complex behavioural and societal factors contribute systemically to the current crisis and no single influence dominates.555CD992, 399972Impacts of obesityObesity presents a significant threat to the health of the UK population and a significant drain on the nation's financial resources. 23% of adults are obese—with a body mass index of over 30—61% of adults are either overweight or obese (with a BMI of over 25), and 33% of 10–11-year-olds are overweight or obese. The annual cost of obesity to the UK economy has been estimated to be £27bn–£46bn [1], [2]; although international comparisons suggest that the true cost could be significantly higher.57DE7179, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179, 399984Inequality of impactAlthough obesity occurs across all population groups, it impacts disproportionately on the socially and economically disadvantaged and some ethnic minorities. [8]57DE7179 URL:
|
Link[4] Tackling Obesity in England
En citant: National Audit Office
Publication info: 2001 February, 15
Cité par: David Price 4:03 PM 7 September 2014 GMT
Citerank: (2) 349156National Audit OfficeThe National Audit Office (NAO) scrutinises public spending on behalf of Parliament. Our audit of central government has two main aims. By reporting the results of our audits to Parliament, we hold government departments and bodies to account for the way they use public money, thereby safeguarding the interests of taxpayers. In addition, our work aims to help public service managers improve performance and service delivery.58D3ABAB, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179
URL:
| | Extrait - Sir John Bourn, head of the National Audit Office, told Parliament today that the prevalence of obesity in England had tripled over the last 20 years and continues to rise. Most adults in England are now overweight, and one in five is obese.
Producing the first authoritative estimates of the costs and consequences of obesity in England, Sir John estimated that obesity accounted for 18 million days of sickness absence and 30,000 premature deaths in 1998. On average, each person whose death could be attributed to obesity lost nine years of life. Treating obesity costs the NHS at least £½ billion a year. The wider costs to the economy in lower productivity and lost output could be a further £2 billion each year.
Sir John recommends that greater effort is placed on establishing an evidence based approach to the problem to enable the NHS to adopt a more consistent approach to the management of obesity. Continued and more extensive joint working across government is also needed, both nationally and locally, to promote long term changes in lifestyles |
Link[5] Health and economic burden of the projected obesity trends in the USA and the UK
En citant: Y Claire Wang, Klim McPherson, Tim Marsh, Steven L Gortmaker, Martin Brown
Publication info: 2011 August, 27 – The Lancet, Volume 378, Issue 9793, Pages 815 - 825
Cité par: David Price 4:16 PM 7 September 2014 GMT
Citerank: (7) 362031Financial cost of obesity – USAAnalysis [6] prepared for The Fiscal Times by Scott Kahan—director of the National Center for Weight & Wellness at George Washington University—puts the total national cost of obesity (including direct medical and non-medical services, decreased worker productivity, disability and premature death) at $305.1bn annually. Including the intangible costs associated with pain and suffering from obesity and obesity-associated conditions would add at least a further $300bn a year (Society of Actuaries).959C6EF, 366990What costs should be included in the financial analysis?What cost factors should be included in the assessment of the overall financial impact of obesity on the UK economy?8FFB597, 370359Financial cost of obesity – international comparisons8FFB597, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179, 399980What costs should be included in the financial analysis?What cost factors should be included in the assessment of the overall financial impact of obesity on the UK economy?8FFB597, 399981Financial cost of obesity – international comparisons8FFB597, 400007Financial cost of obesity – USAAnalysis [6] prepared for The Fiscal Times by Scott Kahan—director of the National Center for Weight & Wellness at George Washington University—puts the total national cost of obesity (including direct medical and non-medical services, decreased worker productivity, disability and premature death) at $305.1bn annually. Including the intangible costs associated with pain and suffering from obesity and obesity-associated conditions would add at least a further $300bn a year (Society of Actuaries).959C6EF URL:
| | Extrait - Rising prevalence of obesity is a worldwide health concern because excess weight gain within populations forecasts an increased burden from several diseases, most notably cardiovascular diseases, diabetes, and cancers. In this report, we used a simulation model to project the probable health and economic consequences in the next two decades from a continued rise in obesity in two ageing populations—the USA and the UK. These trends project 65 million more obese adults in the USA and 11 million more obese adults in the UK by 2030, consequently accruing an additional 6 – 8·5 million cases of diabetes, 5·7 – 7·3 million cases of heart disease and stroke, 492,000—669,000 additional cases of cancer, and 26 – 55 million quality-adjusted life years forgone for USA and UK combined. The combined medical costs associated with treatment of these preventable diseases are estimated to increase by $48 – 66 billion/year in the USA and by £1·9 - 2 billion/year in the UK by 2030. Hence, effective policies to promote healthier weight also have economic benefits. |
Link[7] Economic costs of obesity and the case for government intervention
En citant: B. McCormick, I. Stone, Corporate Analytical Team
Publication info: 2007 March, Obesity Reviews, Volume 8, Issue Supplement s1, pages 161–164, DOI: 10.1111/j.1467-789X.2007.00337.x
Cité par: David Price 4:46 PM 7 September 2014 GMT
Citerank: (3) 366990What costs should be included in the financial analysis?What cost factors should be included in the assessment of the overall financial impact of obesity on the UK economy?8FFB597, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179, 399980What costs should be included in the financial analysis?What cost factors should be included in the assessment of the overall financial impact of obesity on the UK economy?8FFB597
URL:
| | Extrait - Obesity imposes a significant human burden of morbidity, mortality, social exclusion and discrimination. There is also a significant healthcare cost associated with treating obesity and its direct consequences. And social care costs are higher for the obese. Higher levels of sickness and absence from work among the obese reduce productivity and impose costs on businesses. Premature mortality as a consequence of obesity reduces the national output relative to the level it would be in the absence of obesity.
Obesity also imposes other costs. Many people are not in employment as a direct result of obesity, either on health grounds or for other reasons, including, possibly, discrimination in the workforce. This, too, reduces national output, reduces tax revenue and increases government expenditure on incapacity benefit and unemployment benefit. In addition, obesity increases operating costs for some businesses, for example, the costs of larger seats and fuel for aircraft. |
Link[8] Tackling obesity: all talk, no action
En citant: HOOP
Publication info: 2014 March, 10
Cité par: David Price 3:00 PM 8 September 2014 GMT
Citerank: (6) 348688Impacts of obesityObesity presents a significant threat to the health of the UK population and a significant drain on the nation's financial resources. 24.9% of adults in England are obese—with a body mass index of over 30—62% of adults are either overweight or obese (with a BMI of over 25), and 32% of 10–11-year-olds are overweight or obese. The annual cost of obesity to the UK is estimated to be £27bn–£46bn [1], [2]; although international comparisons suggest that the true cost could be significantly higher.57DE7179, 349155HOOP UKHOOP UK aims to be the 'go to’ organisation in the UK for support for those struggling with the issues surrounding weight management and obesity.58D3ABAB, 352558Giving obesity a disproportionately low public health priority555CD992, 399905Giving obesity a disproportionately low public health priority555CD992, 399972Impacts of obesityObesity presents a significant threat to the health of the UK population and a significant drain on the nation's financial resources. 23% of adults are obese—with a body mass index of over 30—61% of adults are either overweight or obese (with a BMI of over 25), and 33% of 10–11-year-olds are overweight or obese. The annual cost of obesity to the UK economy has been estimated to be £27bn–£46bn [1], [2]; although international comparisons suggest that the true cost could be significantly higher.57DE7179, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179
URL: | | Extrait - 1 in 3 children and 2 in 3 adults are overweight and obese. The estimated annual cost of obesity to this country is £27bn which is very high considering the annual interest on our national debt are £43bn.
Key Findings
Based on the 109 local authorities that responded to the Freedom of Information request submitted by HOOP UK, it was identified that:
> 2.5% of the public health allocation was spent on weight management services
> 0.9% of the allocation was spent on children’s weight management services
> These allocations are extremely low compared to: Substance misuse (29%) Sexual Health (21%) and Smoking (5%)
This disparity is more problematic when the direct and indirect costs of each public health issue are considered: Obesity (£6.1bn (direct) and £27bn (indirect); Drugs misuse (£488m and £14.9bn); Alcohol misuse(£3.5bn and £21bn) and sexual health (£1.5bn and £14.1bn) respectively. |
Link[9] The economic burden of obesity worldwide: a systematic review of the direct costs of obesity
En citant: D. Withrow, D.A. Alter
Publication info: 2011 February, Obes Rev. 2011 Feb;12(2):131-41. doi: 10.1111/j.1467-789X.2009.00712.x.
Cité par: David Price 8:05 AM 9 September 2014 GMT
Citerank: (7) 362031Financial cost of obesity – USAAnalysis [6] prepared for The Fiscal Times by Scott Kahan—director of the National Center for Weight & Wellness at George Washington University—puts the total national cost of obesity (including direct medical and non-medical services, decreased worker productivity, disability and premature death) at $305.1bn annually. Including the intangible costs associated with pain and suffering from obesity and obesity-associated conditions would add at least a further $300bn a year (Society of Actuaries).959C6EF, 366990What costs should be included in the financial analysis?What cost factors should be included in the assessment of the overall financial impact of obesity on the UK economy?8FFB597, 370359Financial cost of obesity – international comparisons8FFB597, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179, 399980What costs should be included in the financial analysis?What cost factors should be included in the assessment of the overall financial impact of obesity on the UK economy?8FFB597, 399981Financial cost of obesity – international comparisons8FFB597, 400007Financial cost of obesity – USAAnalysis [6] prepared for The Fiscal Times by Scott Kahan—director of the National Center for Weight & Wellness at George Washington University—puts the total national cost of obesity (including direct medical and non-medical services, decreased worker productivity, disability and premature death) at $305.1bn annually. Including the intangible costs associated with pain and suffering from obesity and obesity-associated conditions would add at least a further $300bn a year (Society of Actuaries).959C6EF URL: | | Extrait - In the last decade, the prevalence of obesity has increased significantly in populations worldwide. A less dramatic, but equally important increase has been seen in our knowledge of its effects on health and the burden it places on healthcare systems. This systematic review aims to assess the current published literature on the direct costs associated with obesity. A computerized search of English language articles published between 1990 and June 2009 yielded 32 articles suitable for review. Based on these articles, obesity was estimated to account for between 0.7% and 2.8% of a country's total healthcare expenditures. Furthermore, obese individuals were found to have medical costs that were approximately 30% greater than their normal weight peers. Although variations in inclusion/exclusion criteria, reporting methods and included costs varied widely between the studies, a lack of examination of how and why the excess costs were being accrued appeared to be a commonality between most studies. Accordingly, future studies must better explore how costs accrue among obese populations, in order to best facilitate health and social policy interventions. |
Link[11] Overcoming obesity: An initial economic analysis
En citant: Richard Dobbs, Corinne Sawers, Fraser Thompson, James Manyika - Jonathan Woetzel, Peter Child, Sorcha McKenna, Angela Spatharou (McKinsey Global Institute)
Publication info: 2014 November
Cité par: David Price 7:31 PM 30 November 2014 GMT
Citerank: (60) 340964Tackling obesity in the UKWith concern growing that the Foresight analysis—that 50% of the UK population could be obese by 2050, at an annual cost to the nation of around £50 billion per year [2]—substantially underestimates the scale of the unfolding obesity crisis, the College of Contemporary Health is working with the wider policy community to develop a whole systems map of the obesity crisis and the potential responses.7F1CEB7, 348675Adopt a whole systems approach to obesityTackling obesity effectively—accomplishing a population wide-shift—requires a comprehensive and integrated whole systems approach, involving a range of measures focusing on individuals, social and other systems, including at the local and community level, and on the interrelated physical, physiological, social and cognitive factors that determine health outcomes.565CA4D9, 348770Tackling obesityMany policy interventions have been suggested to address the obesity crisis across multiple studies—and indeed many such measures have been implemented, and are being implemented, now. There's recognition too that these interventions need to be part of a coherent and comprehensive whole systems strategy [4]; with some grounds for optimism that such an approach has the potential to accomplish a significant reduction in the prevalence of obesity in the UK across the next decade. [2]565CA4D9, 348780Causes of obesityUnderstanding the causes of obesity is critical to the success of prevention and treatment strategies. However, while (simply put) obesity occurs when energy intake from food and drink consumption is greater than energy expenditure through the body’s metabolism and physical activity over a prolonged period (resulting in the accumulation of excess body fat), in reality many complex behavioural and societal factors contribute systemically to the current crisis and no single influence dominates.555CD992, 352311Lost productivityObesity has as a serious impact on UK economic development – constraining economic productivity and increasing business costs – affecting individuals’ ability to get and hold down work, their self-esteem and their underlying mental health.57DE7179, 352311Lost productivityObesity has as a serious impact on UK economic development – constraining economic productivity and increasing business costs – affecting individuals’ ability to get and hold down work, their self-esteem and their underlying mental health.57DE7179, 352373Invest in weight management servicesThe departments of health in the four nations should extend and increase the provision of weight management services across the country, to mirror the provision of smoking cessation services.565CA4D9, 352710Develop better pharmaceutical obesity therapiesObesity drug sales are forecast to $3.8bn globally in 2018 [2]—in comparison to $57bn for Diabetes drug sales[2]—with evidence suggesting that the modest average weight losses achieved with current anti-obesity agents may be of some clinical benefit [5]. However, the current generation of drugs, which act on the central nervous system to suppress appetite, have raised significant health concerns—including psychiatric disorders, such as suicidal behaviour, depression, and cardiovascular problems.565CA4D9, 352718Invest in employee health and wellbeingEncourage organisations to invest employee health and wellbeing; including a health risk assessment and the provision of resources to help employees address the factors that pose the greatest risk to their health and wellness. [1], [2], [3], [4], [5]565CA4D9, 366161McKinsey Global InstituteThe MGI discussion paper, Overcoming obesity: An initial economic analysis studied studied 74 interventions (in 18 areas) that are being discussed or piloted somewhere around the world to address obesity, including subsidized school meals for all, calorie and nutrition labeling, restrictions on advertising high-calorie food and drinks, and public-health campaigns – with sufficient data found on 44 of the interventions in 16 areas. 58D3ABAB, 366169Obesity Interventions identified by MGI74 interventions – across 18 groups – to reduce obesity.565CA4D9, 366449Deploy and integrate as many interventions as possible at scaleCommission and deploy as many interventions as possible at scale and delivered effectively, and integrated way, by the full range of sectors in society.565CA4D9, 366450Understand how to align incentives and build cooperation109FDEF6, 366452No single solution creates sufficient impact to reverse obesityNo single solution creates sufficient impact to reverse obesity: only a comprehensive, systemic program of multiple interventions is likely to be effective. 1198CE71, 366453Many interventions are highly cost-effectiveAlmost all of the interventions we analyzed are highly cost-effective from the viewpoint of society.1198CE71, 366454Education and personal responsibility are necessary but not sufficientEducation and encouraging personal responsibility are necessary but not sufficient.1198CE71, 366456Co-ordinated multi-party actions are required to tackle obesityCapturing the full potential impact is likely to require commitment from government, employers, educators, retailers, restaurants, and food and beverage manufacturers, and a combination of top-down corporate and government interventions and bottom-up community-based ones. 1198CE71, 366457Government obesity efforts are too fragmented to be effectiveGovernment efforts to tackle the obesity issue seem too fragmented to be effective. In the United Kingdom, 15 central government departments; all local authorities with responsibility for health, education, and local planning; 16 EU directorates-general; and a wide range of nongovernmental organizations all have a significant impact on the major intervention areas. [1]118FF4888, 366458Current incentives are mis-aligned118FF4888, 366460Desire to prioritise options becomes a barrier to actionA search for the “best” interventions or a single solution could delay action and displace responsibility. Given the seriousness of the obesity issue, the aim should be to do as much as possible as soon as possible. [1]118FF4888, 366462Experiment with multiple interventionsSociety should be prepared to experiment with possible interventions. In many intervention areas, impact data from high-quality, randomized control trials are not possible to gather. So, rather than waiting for such data, the relevant sectors of society should be pragmatic with a bias toward action, especially where the risks of intervening are low, using trial and error to flesh out their understanding of potential solutions. 565CA4D9, 366463Paucity of investment in intervention measuresThe UK invests less than $1 billion a year in prevention activities such as weight-management programs and public health campaigns – i.e. around 1% of the social cost of obesity in the UK. More investment is required.555CD992, 366467Encourage active transport (walking and cycling)Government authorities redesign urban planning to facilitate and encourage walking and cycling.565CA4D9, 366479Align the school curriculum with obesity, nutrition and activity goals565CA4D9, 366479Align the school curriculum with obesity, nutrition and activity goals565CA4D9, 366481Improve surgical interventions for obesity565CA4D9, 366483Types of weight-management services565CA4D9, 366555Employers offer team challenge incentive schemes in the workplaceEmployers provide team challenge activities to encourage physical activity and improved key health indicators in the workplace.565CA4D9, 366557Employers give employees financial incentives to improve healthEmployers provide material incentives to individuals for improved key health indicators (e.g., discounts on insurance premiums, gym membership, prizes).565CA4D9, 366827Develop a coherent fiscal, regulatory and governance frameworkTake every opportunity, iteratively over time, to bring the public fiscal, regulatory and governance framework into alignment with public health goals on obesity. Use taxes, subsidies, targets and pricing signals to incentivise change in behaviour, supply and consumption by aligning measures with the health properties of food and drink and behaviour—and seek, wherever practical, to amplify positive patterns that are aligned with the policy goals and damp those that pull against.565CA4D9, 371556Many obesity policy measures appear to be cost-effective for societyThe recent MGI study [1] reported that almost all of the obesity policy interventions included in its economic analysis appeared to be highly cost-effective at the societal level—i.e. the health-care costs and productivity savings that accrue from reducing obesity through a specific intervention outweighed the direct investment required to deliver that intervention when assessed over the full lifetime of the target population.1198CE71, 399546Tackling obesityMany policy interventions have been suggested to address the obesity crisis across multiple studies—and indeed many such measures have been implemented, and are being implemented, now. There's recognition too that these interventions need to be part of a coherent and comprehensive whole systems strategy [4]; with some grounds for optimism that such an approach has the potential to accomplish a significant reduction in the prevalence of obesity in the UK across the next decade. [2]565CA4D9, 399547Adopt a whole systems approach to obesityTackling obesity effectively—accomplishing a population wide-shift—requires a comprehensive and integrated whole systems approach, involving a range of measures focusing on individuals, social and other systems, including at the local and community level, and on the interrelated physical, physiological, social and cognitive factors that determine health outcomes.565CA4D9, 399548Invest in employee health and wellbeingEncourage organisations to invest employee health and wellbeing; including a health risk assessment and the provision of resources to help employees address the factors that pose the greatest risk to their health and wellness. [1], [2], [3], [4], [5]565CA4D9, 399552Develop a coherent fiscal, regulatory and governance frameworkTake every opportunity, iteratively over time, to bring the public fiscal, regulatory and governance framework into alignment with public health goals on obesity. Use taxes, subsidies, targets and pricing signals to incentivise change in behaviour, supply and consumption by aligning measures with the health properties of food and drink and behaviour—and seek, wherever practical, to amplify positive patterns that are aligned with the policy goals and damp those that pull against.565CA4D9, 399555Many obesity policy measures appear to be cost-effective for societyThe recent MGI study [1] reported that almost all of the obesity policy interventions included in its economic analysis appeared to be highly cost-effective at the societal level—i.e. the health-care costs and productivity savings that accrue from reducing obesity through a specific intervention outweighed the direct investment required to deliver that intervention when assessed over the full lifetime of the target population.1198CE71, 399561Deploy and integrate as many interventions as possible at scaleCommission and deploy as many interventions as possible at scale and delivered effectively, and integrated way, by the full range of sectors in society.565CA4D9, 399567Employers offer team challenge incentive schemes in the workplaceEmployers provide team challenge activities to encourage physical activity and improved key health indicators in the workplace.565CA4D9, 399568Employers give employees financial incentives to improve healthEmployers provide material incentives to individuals for improved key health indicators (e.g., discounts on insurance premiums, gym membership, prizes).565CA4D9, 399575Align the school curriculum with obesity, nutrition and activity goals565CA4D9, 399575Align the school curriculum with obesity, nutrition and activity goals565CA4D9, 399586Develop better pharmaceutical obesity therapiesObesity drug sales are forecast to $3.8bn globally in 2018 [2]—in comparison to $57bn for Diabetes drug sales[2]—with evidence suggesting that the modest average weight losses achieved with current anti-obesity agents may be of some clinical benefit [5]. However, the current generation of drugs, which act on the central nervous system to suppress appetite, have raised significant health concerns—including psychiatric disorders, such as suicidal behaviour, depression, and cardiovascular problems.565CA4D9, 399588Improve surgical interventions for obesity565CA4D9, 399592Invest in weight management servicesThe departments of health in the four nations should extend and increase the provision of weight management services across the country, to mirror the provision of smoking cessation services.565CA4D9, 399599Encourage active transport (walking and cycling)Government authorities redesign urban planning to facilitate and encourage walking and cycling.565CA4D9, 399611Understand how to align incentives and build cooperation109FDEF6, 399612Co-ordinated multi-party actions are required to tackle obesityCapturing the full potential impact is likely to require commitment from government, employers, educators, retailers, restaurants, and food and beverage manufacturers, and a combination of top-down corporate and government interventions and bottom-up community-based ones. 1198CE71, 399613No single solution creates sufficient impact to reverse obesityNo single solution creates sufficient impact to reverse obesity: only a comprehensive, systemic program of multiple interventions is likely to be effective. 1198CE71, 399614Many interventions are highly cost-effectiveAlmost all of the interventions we analyzed are highly cost-effective from the viewpoint of society.1198CE71, 399615Education and personal responsibility are necessary but not sufficientEducation and encouraging personal responsibility are necessary but not sufficient.1198CE71, 399617Experiment with multiple interventionsSociety should be prepared to experiment with possible interventions. In many intervention areas, impact data from high-quality, randomized control trials are not possible to gather. So, rather than waiting for such data, the relevant sectors of society should be pragmatic with a bias toward action, especially where the risks of intervening are low, using trial and error to flesh out their understanding of potential solutions. 565CA4D9, 399715Types of weight-management services565CA4D9, 399887Causes of obesityUnderstanding the causes of obesity is critical to the success of prevention and treatment strategies. However, while (simply put) obesity occurs when energy intake from food and drink consumption is greater than energy expenditure through the body’s metabolism and physical activity over a prolonged period (resulting in the accumulation of excess body fat), in reality many complex behavioural and societal factors contribute systemically to the current crisis and no single influence dominates.555CD992, 399932Paucity of investment in intervention measuresThe UK invests less than $1 billion a year in prevention activities such as weight-management programs and public health campaigns – i.e. around 1% of the social cost of obesity in the UK. More investment is required.555CD992, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179, 400018Lost productivityObesity has as a serious impact on UK economic development – constraining economic productivity and increasing business costs – affecting individuals’ ability to get and hold down work, their self-esteem and their underlying mental health.57DE7179, 400018Lost productivityObesity has as a serious impact on UK economic development – constraining economic productivity and increasing business costs – affecting individuals’ ability to get and hold down work, their self-esteem and their underlying mental health.57DE7179, 400061Current incentives are mis-aligned118FF4888, 400083Government obesity efforts are too fragmented to be effectiveGovernment efforts to tackle the obesity issue seem too fragmented to be effective. In the United Kingdom, 15 central government departments; all local authorities with responsibility for health, education, and local planning; 16 EU directorates-general; and a wide range of nongovernmental organizations all have a significant impact on the major intervention areas.118FF4888, 400084Desire to priortise options becomes a barrier to actionA search for the “best” interventions or a single solution could delay action and displace responsibility. Given the seriousness of the obesity issue, the aim should be to do as much as possible as soon as possible.118FF4888 URL:
|
Link[13] Get serious about obesity or bankrupt the NHS - Simon Stevens
En citant: Simon Stevens - NHS England
Publication info: 2014 September, 17
Cité par: David Price 11:05 AM 21 December 2014 GMT
Citerank: (5) 371552Financial cost of obesity grows as the prevalence of obesity risesThe cost of treating the health consequences of obesity, and productivity losses due to obesity, increase as the prevalence of obesity spreads in the population.1198CE71, 373021Offer tax breaks to firms that incentivise employee healthOffer tax breaks to employers who provide effective NICE-certified workplace health programmes for employees.565CA4D9, 399820Offer tax breaks to firms that incentivise employee healthOffer tax breaks to employers who provide effective NICE-certified workplace health programmes for employees.565CA4D9, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179, 399982Financial cost of obesity grows as the prevalence of obesity risesThe cost of treating the health consequences of obesity, and productivity losses due to obesity, increase as the prevalence of obesity spreads in the population.1198CE71
URL:
|
Link[14] Obesity's Worse than We Thought? Bullshit
En citant: Rob Lyons
Publication info: 2014 January, 13
Cité par: David Price 1:31 AM 3 January 2015 GMT
Citerank: (2) 365986Foresight – Obesity System MapObesity occurs when energy intake from food and drink consumption is greater than energy expenditure through the body’s metabolism and physical activity over a prolonged period, resulting in the accumulation of excess body fat. However there are many complex behavioural and societal factors that combine to contribute to the causes of obesity.7F1CEB7, 399973A potentially unsustainable financial burden on the health systemThe range of obesity's impacts makes accurate economic analysis challenging; however, a November 2014 study from the McKinsey Global Institute placed the annual economic impact on the UK at around $73bn (£46bn). Earlier analysis and modelling for the 2007 Foresight Report suggested a cost to the NHS of around £4.2bn annually to treat people with health problems related to elevated BMI and a total wider cost to the economy of around £15.8bn (rising to £27bn by 2015 and £49.9bn by 2050).57DE7179
URL:
| | Extrait - The claim that more than half of Britons will be obese by 2050 flies in the face of the data...
...the data would suggest that the number of obese adults and children rose sharply in the Nineties and early Noughties, but from then on has plateaued among adults and fallen among children. This should be a moment when we pause and reassess the results of those Foresight models - which, far from understated, looked ludicrous at the time - and ask whether in fact people have got pretty much as fat as they are going to get, at least in countries that have had a spurt in obesity rates in the past 20 years. That would certainly be in keeping with a review of obesity studies from around the world published in Obesity Reviews in 2011, which stated: ‘A literature and internet search resulted in 52 studies from 25 different countries. The findings supported an overall levelling off of the epidemic in children and adolescents from Australia, Europe, Japan and the USA. In adults, stability was found in the USA, while increases were still observed in some European and Asian countries.’ |
|
|